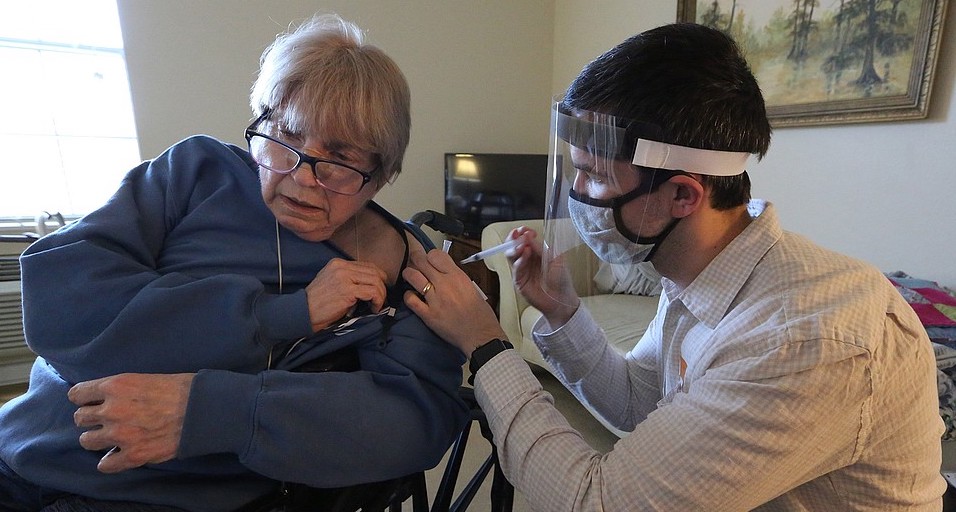
A Pandemic Strikes
A year later, Arkansas covid-19 survivors see ills linger
By Jeannie Roberts
The series “A Pandemic Strikes” will examine covid-19’s impact on the state. This article marks the one-year anniversary of the state’s first confirmed case on March 11, 2020.
Barbara Ritter walked along the planks of the Lake Dardanelle fishing pier toward the gazebo shelter over the water.
Her gait was slow, but this day, strong.
Only two months earlier, Ritter, 52, a covid-19 virus survivor from Ola, couldn’t walk even a few feet without assistance and without her oxygen levels plummeting.
“I never have a day when I feel good. I either feel pretty good, fair or bad,” Ritter said. “I am so sore, and I hurt so badly when I move around that I can’t hardly stand it. I have to take meds and use a heating pad day and night most days.”
Ritter started coughing Aug. 5 and days later was in the hospital on a ventilator fighting for her life. Since then, Ritter has struggled with myriad debilitating lung, heart, skin and neurological issues that her doctors attributed to covid-19.
She is now a member of what is known as “covid long-haulers,” people who have symptoms or other health issues long after the initial covid infection has cleared.
The National Institute of Health just recently named the condition: Post-Acute Sequelae of ARS-CoV-2 Infection or PASC.
While statistics are scarce on the long-term effects of the covid-19 virus, national studies estimate that about a third of survivors have symptoms and other debilitating issues that last long after what is considered “recovered.”
By those numbers, about 106,600 Arkansans — or 33% of the nearly 324,000 cumulative covid cases since the virus officially hit the state a year ago March 11 — struggle with the aftermath of the disease.
“We still have a long way to go when it comes to recovering from this pandemic,” said Dr. Bala Simon, acting chief medical officer of the Arkansas Department of Health.”We are seeing more and more people who have symptoms related to covid past their initial infection.”
The covid-19 illness typically lasts from two to four weeks, Simon said. It’s when symptoms continue past four weeks that the patient is deemed a “covid long-hauler.”

Barbara Ritter, left, and daughter Charity Keener talk about the lasting effects of having covid. (Arkansas Democrat-Gazette/Staton Breidenthal)
For the long haul
While covid-19 largely attacks the lungs, U.S.Centers for Disease Control and Prevention officials say they are learning that many organs are affected by the disease.
The most common lingering symptoms include fatigue, shortness of breath, cough, joint pain and chest pain, but some have reported “brain fog” (difficulty with thinking, memory and concentration), headache, anxiety, depression, muscle pain, intermittent fever, heart palpitations, rash, hair loss, loss of smell and taste, and sleep issues.
Some of the most serious after-effects are blood clots, inflammation of the heart muscle, lung function abnormalities and acute renal injury.
“Some covid-19 patients continue to have symptoms for weeks and months after their initial diagnosis such as persistent fatigue and brain fog that leaves people unable to work,” said Dr. Jennifer Dillaha, state epidemiologist. “While this appears to only affect a small number of patients, it is another distressing aspect of this virus and one that will be important to continue studying, so we can learn more about the cause and potential treatments.”
These persistent effects are not limited to patients who had severe illness, Dillaha added.
“They are sometimes seen in patients who had only mild symptoms initially,” Dillaha said. “This should serve as another reminder that Arkansans need to do everything they can to prevent getting infected or spreading covid-19 because the implications are serious and possibly long-lasting. This means we should wear face masks, maintain physical distance, avoid crowds, wash hands frequently and get the vaccine once it is available.”
The after-effects do not discriminate between the young and the old or those who had mild or severe cases of the virus. In fact, studies are showing that physically fit patients tend to have more severe long-term symptoms.
A Mayo Clinic report estimates that up to 30% of covid-19 long-haulers are debilitated to the point that they had to quit work.
Inflammation throughout the body and its organs is covid-19’s weapon of choice, Simon said.
“What we identified is, since this is a viral infection, there is a post-acute hyper-inflammatory phase,” Simon said. “That’s where we start getting reports of multi-inflammatory syndrome or MIS-C in children.”
The severe inflammation can attack the body’s vital organs, like the heart, brain, kidneys and lungs.
“A post-covid patient can develop shortness of breath related to what we call the ‘covid lung.’ A CAT scan paints a picture similar to the smokers lung of a chronic smoker with some type of fibrosis,” Simon said. “Fibrosis is basically destruction of the lung tissue. The question is whether there was a pre-existing condition that wasn’t diagnosed, then all hell breaks loose when covid hit — or is it something new?”
The biggest problem now is that there is no solid definition of what long-haul covid-19 is, said Dr. Robert Hopkins, an internist at the University of Arkansas for Medical Sciences’ Internal Medicine Clinic in Little Rock.
“It’s a constellation of a number of different symptoms that could result from covid itself or it could be results of people being critically ill and being in intensive care on ventilation and sedating medicine,” Hopkins said. “It could be residual from the damage of your own immune system being overactive. We really don’t know.”
The heart of covid
Before testing positive for covid-19 in August, Barbara Ritter’s only health issue was well-controlled Type 2 diabetes.
She was in the hospital for the first time in her life on Aug. 15, when her covid-19 infection took a turn for the worse.
She had recently retired after more than 26 years as pastor at Cross Connect Outreach Center in Danville and was well into a career as an admissions clerk at the Western Yell County Medical Clinic, a satellite of Chambers Memorial Hospital in Havana.
“She was going strong from the break of dawn until she went to bed that night,” said her daughter, Charity Keener.
As a three-time Arkansas Game and Fish Commission Master Angler, Ritter was always out casting a line. She gardened and donated the harvest and other necessities to the elderly. She is a master seamstress and regularly played the piano, guitar and drums. She frequently remodeled her home and those of others, building cabinets and adding rooms.
When she was weaned off the ventilator and heading home Aug. 25, dozens of health care workers at the Conway Regional Hospital lined the hallway cheering her as a “miracle.”
“I had been on the bottom, so I figured up was the only direction to go,” Ritter said.
Ritter was on supplemental oxygen at home. When she tried to walk, she gasped for breath and her oxygen levels dropped.
“It took about a month before she could walk through the house unassisted,” Keener said.
Keener tested positive for covid-19 within days of her mother’s diagnosis, but recovered quickly. She has no major long-term effects other than her senses of taste and smell “still aren’t right.”
Ritter has been to a multitude of doctors and specialists, and has ended up in the emergency room several times since she was first diagnosed.
She’s unable to work, or attend church since the effort it takes to get “church-ready” takes too great a toll on her system.
“From the time she got home from the hospital, for months, she would suddenly have hard and frequent involuntary muscle jerks and her body would vibrate so hard she would shake the furniture she was on,” Keener said. “This was worse if she was fatigued.”
Ritter developed inflammation of the optical nerves, compromising her vision. She lost a third of her hair. Her once-smooth skin is now chronically dry. Ritter is just now beginning to recover her sense of smell.
Her glucose levels have skyrocketed and are hard to manage.
“She’s finally able to get it down to 200, which still isn’t great,” Keener said. “Covid hit her pancreas hard.”
Ritter is exhausted most days. She has chronic insomnia that is resistant to medication; she finally falls asleep between 3 a.m. to 5 a.m. each day.
“The right quarter of my head was numb,” Ritter said. “There was no pain. It was just numb for about two months. Yesterday, that exact same area was tingling.
“I can only read for small amounts at a time. My mind gets exhausted because I have trouble thinking and comprehending what I read. This is a big deal because I used to study 12-18 hours a day when I pastored.”
The covid brain fog persists, leaving her grasping desperately for words and struggling to remember what happened 30 minutes ago.
“I pushed myself to walk and to drive. I wasn’t comfortable driving because my head hurt. People like me are referred to as long-haulers. I don’t like the term, but it is what it is,” Ritter said. “I had such a brain fog that I couldn’t remember anything. I would ride down the road with Charity driving, and I would follow that, but I didn’t feel like I was safe from myself, and others weren’t safe from me on the road. My thinking wasn’t clear, wasn’t sharp enough, it wasn’t quick enough.”
Heart damage
On Nov. 19, Ritter had a regular pulmonary function test that required her to quickly and forcibly expel breath through tubes.
Afterward, sharp pains radiated down her left arm.
Ritter — who had never had heart problems previously or any blood work indicating risks — had triple bypass surgery on Jan. 6.
“She had no plaque. Zero,” Keener said. “The doctor said it was all scar tissue and inflammation from covid.”
A recent Journal of the American Medical Association study found heart abnormalities in 78% of 100 people studied who had recovered from covid-19. The culprit is cardiac inflammation caused by the virus.
Many of the study participants had indicators of scarring and decreased right ventricle function.
Today, Ritter walks for longer intervals and drives short distances. And she’s determined to get back to her favorite fishing hole.
She doesn’t know what’s down the road or if she will ever fully recover.
“My God is faithful and though I faced all I have, He has been good to me and met my needs. My joy isn’t based on my circumstances, it is based on who God is,” Ritter said. “I deal with depression and anxiety, but I have learned to encourage myself in the Lord, and I have an awesome support team of prayer warriors and friends. They are here for me day and night. I am grateful.”
A year ago
The first weekend in March last year, Alyssa Fuller, 35, a Little Rock wife and mother of two, woke up with a “little tickle” in her throat.
“I felt like I was about to get a cold,” she said. “I had just flown to Denver, and the person on the plane cater-corner of me was coughing the whole time. This was before masks. There were a couple of cases [in the nation], and it was right around the time the first case had popped up in Denver.”
Her fever climbed to 105. She had chills and then lost her sense of smell.
Her husband and both of her girls, 10 and 5, had the same symptoms.
None of them were ever hospitalized for the virus, and they recovered within three weeks of the onset of symptoms.
“Over the course of the next couple of months, I started having desperate, strange symptoms,” she said. “I was waking up to pee about five to six times at nights. I was wheezing and needed an inhaler and [feeling] nauseous. I had trouble ending sentences. I would see a doorknob, but couldn’t get the word out.”
Fuller went to five doctors overall, trying to find the source of her symptoms.
None had answers.
Little was known about covid-19 at the time, and there was no documentation on what happens after the initial infection.
Before covid, Fuller had mild asthma, but no other health issues. Other than for childbirth, she has never been hospitalized.
A year later, Fuller still struggles with kidney, lung and neurological issues.
“The lung stuff is straightforward, but it’s the only thing I’m able to treat successfully,” she said. “That treatment is a $300 a month preventative inhaler — the cheapest option covered by my insurance.”
Fuller’s mother, Pat Ulrich, contracted covid-19 shortly after Fuller. The 57-year-old had high blood pressure as well as asthma.
Ulrich was active and social.
“She got out more than I did,” Fuller said.
After covid, though, Ulrich’s energy disappeared, her breathing was labored and she developed stage three kidney disease.
On Dec. 23, Ulrich was enjoying an early Christmas dinner with her family and died from a heart attack.
Fuller said her fear level about the future is “pretty high.”
“I’m concerned that it’s all going to crop up again, that I’m going to have an issue down the road,” she said. “Am I more susceptible to other things now? Out of all the doctors I’ve talked to, they were like, ‘I don’t know.’”

Alyssa Fuller discusses the complications and symptoms she still has to deal with a year after having covid-19. (Arkansas Democrat-Gazette/Staton Breidenthal)
The future
In December, Congress allocated $1.15 billion over four years for the National Institute of Health to bankroll research on the long-term impact of covid-19.
“We do not know yet the magnitude of the problem, but given the number of individuals of all ages who have been or will be infected with SARS-CoV-2, the coronavirus that causes COVID-19, the public health impact could be profound,” Dr. Francis Collins, NIH director, said in a news release late last month.
In Arkansas, health leaders like UAMS and Arkansas Children’s Hospital have ongoing covid-19 studies, but none that focus on long-term effects.
“We have several studies we are looking at,” said Dr. Jessica Snowden, Arkansas Children’s Hospital’s chief of infectious diseases. “We will make sure we advertise those to our communities. We want to be able to help and get answers.”
Ritter and Fuller say they would welcome the opportunity to participate in covid-19 medical studies.
“Covid has definitely brought everything into sharp relief of how dangerous it is. It’s literally costing people their lives,” Fuller said. “I would love to be a part of the studies and help others.”
Around the nation, some medical providers are working to carve out a path for treating covid-19 long-haulers where there is no standard of care nor national guidelines.
A recent NBC News project identified 80 medical clinics that specifically treat covid-19 patients with continuing symptoms long after the initial infections clear.
One of those clinics was in Arkansas: Medical Associates of Northwest Arkansas, an independent physician group that includes family medicine, pediatrics, women’s health, and several specialists and advanced health services.
The post-covid program is a work in progress and not fully off the ground, said Dr. Allen Moseley, a pulmonologist on the group’s board of directors.
“We noticed the need almost right away,” Moseley said. “We had all these patients who would recover from covid, but then continue to have significant difficulties.”
Covid long-haulers are initially screened by their primary care doctors and referred to the covid program. From there, the patients are scheduled with different specialists, depending on their symptoms and issues.
“The real idea behind the program is to try to streamline the referral process so these people don’t get lost out in the world. Long-haulers have this sense of abandonment,” Moseley said. “They feel like the medical community can’t take care of them. And that’s probably true to an extent. We’re still trying to deal with the actual pandemic and these folks that have survived their hospital stay, but are still sick, are really kind of left in the lurch.”
When word leaked that the post-covid clinic was in the works, Moseley said the response from covid long-haulers was overwhelming.
“I think there’s a pent-up need out there. We’re going to be very busy,” he said. “I think the bigger issue is people really didn’t know what they needed; they just knew they needed something. There’s all these people out there who are still struggling.”
The majority of long-haulers are young, “folks that had jobs and kids and were healthy.”
“They’re not your typical 70-, 80-, 90-year-olds. Those folks, we kind of anticipated they would have problems, but these are young people,” Moseley said. “That really is concerning and worrisome. We hope, as we get them in, we can figure out why we’re seeing so much of this. As of right now, we don’t really know. What we do know is that these people need somewhere to go.”
Fuller said she hopes that more people will come to understand that covid-19 is not just about loss of life.
“It’s about the quality of life for survivors, too,” Fuller said. “There’s so much we don’t know, which means there are many more people like me who are suffering, too. We may have lived through it, but this virus harmed us in ways that we can’t seem to heal from.”
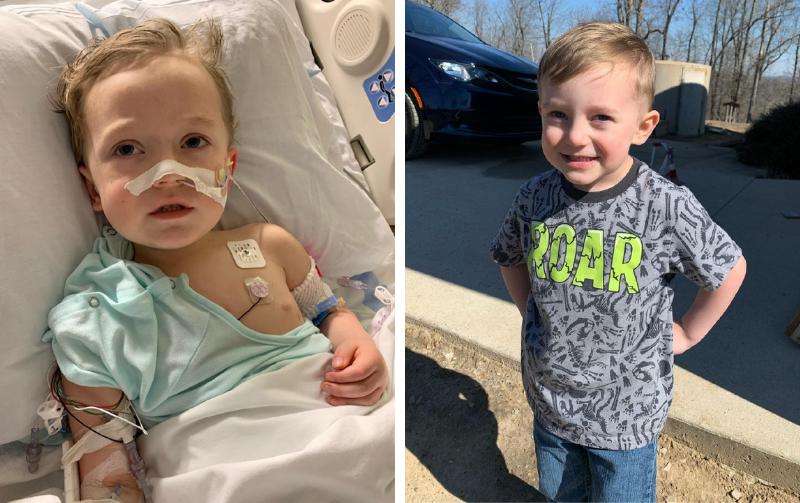
Ollie Rodgers, 4, fell ill on Jan. 2 and days later was fighting for his life at Arkansas Children's Hospital. (Special to the Arkansas Democrat-Gazette)
Virus’s effects in children still an unknown
Whitney and Devin Rodgers were out of the country in early January when they got a frantic call from their home in Baxter County.
Their 4-year-old son, Ollie, was sick. Kim Morrow, Whitney’s mother told them Ollie was lethargic and wouldn’t eat.
That was a Wednesday. By Saturday, Ollie was rushed from Baxter Regional Medical Center in Mountain Home to Arkansas Children’s Hospital in Little Rock.
“He was unresponsive,” Whitney said.
At the hospital, Ollie tested positive for covid-19 and for spinal meningitis.
“It was super scary,” Whitney said.
As the Rodgerses were flying back from a business trip to Mexico, Whitney pleaded on Facebook for prayers for Ollie.
“We had people praying from all over the country and the world,” she said. “His story reached everywhere.”
Since the pandemic hit the state last March, nearly 47,000 children 17 years old and under in Arkansas have contracted the virus.
That’s nearly 14.5% of the state’s nearly 324,000 cumulative cases.
Young adults age 18-24 make up for about 42,000 more cases.
Nationally, about 2.5 million children 17 years old and under — or 11% of about 29 million total cases — have tested positive for the virus.
After weeks in the hospital, Ollie survived his ordeal and is now under the care of specialists at Children’s Hospital monitoring and treating his lingering aftereffects.
No Arkansas children have died directly from covid-19, but some have died from the aftereffects, said Dr. Jessica Snowden, chief of infectious disease at Children’s Hospital.
“We’re seeing them after they’ve had covid — whether they realized they had it, and it has caused problems with their heart, with their stomach,” Snowden said.
While research is limited on covid-19’s long-term effects in children, a main ailment is Multisystem Inflammatory Syndrome in Children, or MIS-C, said Dr. Bala Simon, acting chief medical officer of the Arkansas Department of Health.
And, in children, MIS-C hits the heart hard.
“Covid causes inflammation of the heart muscle, and we’re seeing this more on the younger ages than the older ages,” Simon said.
Simon said the Health Department has sent guidance to providers around the state that it is vital for children to be screened by their doctors before participating in organized sports.
Medical providers should screen for increased heart rate and follow up with an EKG, Simon said.
Snowden agreed.
“We want to make sure they’re cleared before they go back to sports,” Snowden said. “We worry about their heart and the long-term effects.”
MIS-C, according to the CDC, is a condition where different body parts — such as the heart, lungs, kidneys, brain, skin, eyes or gastrointestinal organs — become inflamed after a covid-19 diagnosis.
MIS-C is similar to Kawasaki disease, which primarily affects children, in that both diseases are inflammatory conditions. Kawasaki disease, however, causes swelling in the walls of medium-sized arteries throughout the body.
According to the Centers for Disease Control and Prevention, symptoms of MIS-C include fever, abdominal pain, throwing up, diarrhea, neck pain, rash, bloodshot eyes and feeling extra tired. More severe symptoms include trouble breathing, confusion, inability to wake or stay awake, severe abdominal pain, pain or pressure in the chest that does not go away, and pale-gray or blue skin, lips or nail beds.
Snowden said they’re seeing MIS-C within a few weeks after the initial covid-19 infection.
“Some kids will have fatigue and body aches after covid, just like we see with other viral illnesses,” she said. “We see a wide spectrum of things, and we’re still trying to figure out what all happens long-term.”
Whitney Rodgers said doctors suspect that Ollie’s meningitis was a result of MIS-C.
“One of the thoughts was that covid weakened him enough that the bacteria that causes meningitis got through,” she said.
Meningitis is a neurological disease that causes inflammation of the fluid and membranes surrounding the brain and spinal cord. According to the CDC, such a bacterial or viral infection usually causes the swelling.
Ollie’s parents, as well as his grandmother, tested positive for covid-19 shortly after Ollie was diagnosed. All have recovered.
Ollie is on a daily antibiotic and is improving rapidly. He is being monitored at Arkansas Children’s Hospital and requires speech, occupational and physical therapy. His parents have taken his older brother, Dexter, 7, out of school and are teaching him virtually to reduce the threat of outside bacteria entering the home.
“We’re so grateful he is a fighter,” Whitney said.
On March 2, the National Institute of Health announced a new research effort on how covid-19 affects children, with a focus on the long-term outcomes of MIS-C.
“While much of the devastation wrought by COVID-19 is on older and vulnerable populations, it is affecting children in ways we are just beginning to understand. That’s why this research and these networks are so critical,” said Dr. Gary Gibbons, director of the National Heart, Lung and Blood Institute and co-chair of the NIH initiative.
Arkansas Children’s Hospital will be a part of the studies on long-term covid-19 affects in children, Snowden said.
“It’s just going to take time and keeping an eye on your heart and making sure everything turns out OK. We don’t have a treatment for long-term covid or treatment for symptoms that occur late,” Snowden said. “That’s why it’s so important that we get everybody vaccinated so we can get rid of this. What we’re seeing in symptoms, it may be the tip of the iceberg.”