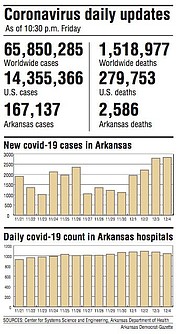
Arkansas' count of coronavirus cases rose Friday by more than 2,800, setting a new high for the second day in a row as the state submitted its order for the first allocation of a vaccine scheduled for review by a federal advisory panel next week.
The death toll from the virus, as tracked by the state Department of Health, rose by 31, to 2,586.
Meanwhile, the number of patients hospitalized in the state with covid-19 fell for the second-straight day, dropping by 31, to 1,041.
Those patients included 191 on ventilators, up from 190 a day earlier.
"We are at a critical point in combating this virus as we continue to see record numbers of new cases each day," Gov. Asa Hutchinson said in a statement.
[CORONAVIRUS: Click here for our complete coverage » arkansasonline.com/coronavirus]
"This battle will not be won by the actions of a few; it will take each Arkansan doing our part to win this fight."
Under the order submitted by the Health Department to the U.S. Centers for Disease Control and Prevention, 17 hospitals and five pharmacies are scheduled to get the first allocation of the vaccine developed by the American drug company Pfizer and its German partner BioNTech.
State Epidemiologist Jennifer Dillaha said the allocation will be directed primarily to hospital workers, with acute-care hospitals with at least 1,000 employees receiving direct shipments.
Because the smallest amount of vaccine that can be shipped from the manufacturer is 975 doses, the five pharmacies will deliver the vaccine to smaller hospitals, she said.
"We have chosen to prioritize hospital workers in order to help support the hospitals and their staffing at this time," Dillaha said.
"Of course, those are the people at highest risk for exposure and infection, and it's at a point in time when the hospitals really can hardly afford to have anyone out for either covid-19 or quarantine."
The Health Department also will receive some of the initial allocation.
[Interactive Arkansas map not showing up above? Click here to see it: arkansasonline.com/arvirus]
"We are going to vaccinate some of our front-line workers in our local health units around the state that do a lot of covid testing as well as will be providing covid vaccinations," Dillaha said.
The initial allotment, expected to be about 25,000 doses, won't be enough for all of the state hospital employees, so hospitals will have to decide which employees receive it first, she said.
"It's our goal to provide some to all the hospitals," Dillaha said.
"We aren't quite sure how the allocations will work out with the smaller hospitals, but that is our goal, to make sure that the highest-risk workers in each hospital get vaccinated."
Meanwhile, the state's initial allocation of a vaccine developed by Massachusetts-based Moderna, if granted an emergency-use authorization by the U.S. Food and Drug Administration, will go to nursing-home residents and workers, Dillaha said.
That's because while the Pfizer vaccine must be stored at temperatures of minus-94 degrees Fahrenheit, the Moderna vaccine can be kept in a standard freezer.
After thawing, it can be kept in a refrigerator for up to 30 days.
"That gives the long-term care pharmacies that are doing the vaccination much more flexibility," Dillaha said.
The minimum shipment for the Moderna vaccine is also smaller -- 100 doses -- making it easier to distribute.
Pfizer's request for an emergency authorization for its vaccine is scheduled to go before an FDA advisory panel Thursday.
If cleared by the FDA, Dillaha said she expects the state to receive its first doses the following week.
That's the same week the Moderna's application will be discussed by the FDA committee, on Dec. 17.
As the state receives more shipments, Dillaha said, vaccinations will be expanded to the rest of the state's highest priority group.
That includes other types of health care workers as well as workers and residents of other types of long-term care facilities, such as assisted-living facilities and centers for people with severe developmental disabilities.
In prioritizing health care workers and long-term care residents, the state followed this week's recommendation of a CDC advisory committee, led by Arkansas Health Secretary Jose Romero, that was then approved by the CDC.
The committee has not yet made a recommendation on who would be next in line, although Romero has said it will likely include "essential personnel" such as teachers and prison workers.
He has said he doesn't expect the state to have enough vaccine for everyone who wants it until the spring or summer.
The hospitals set to receive the initial allotment of vaccine are: Baptist Health-Little Rock; UAMS Medical Center in Little Rock; St. Bernards Medical Center in Jonesboro; CHI St. Vincent-Little Rock; Washington Regional Medical Center in Fayetteville; Mercy Hospital in Fort Smith; Baptist Health-Fort Smith; White River Medical Center in Batesville; Conway Regional Medical Center; Mercy Hospital in Rogers; Baptist Health-North Little Rock; Jefferson Regional Medical Center in Pine Bluff; CHI St. Vincent-Hot Springs; Unity Health-White County Medical Center in Searcy; Baxter Regional Medical Center in Mountain Home; Northwest Medical Center in Springdale; and Arkansas Heart Hospital in Little Rock.
Westside Pharmacy in Benton; Woodsprings Pharmacy in Jonesboro; Kavanaugh Pharmacy in Little Rock; Village Healthmart Pharmacy No. 1 in Hot Springs Village; and Hyde Pharmacy in Paragould will distribute the vaccine to smaller hospitals.
Dillaha said the Health Department worked with the Arkansas Pharmacists Association to identify pharmacies that were willing to provide the vaccinations, had the capacity to store it and had experience administering vaccines.
RECORD ACTIVE CASES
The rise of 2,827 cases in Arkansas on Friday followed an increase of 2,789 a day earlier.
Before those two spikes, the record for a one-day increase was the 2,348 cases on Nov. 26.
Over a rolling seven-day period, the average number of cases added each day hit a new high Friday as it rose by 254, to 1,923.
With new cases outpacing recoveries, the number of cases that were considered active also set a record, as it rose by 923, to 18,032.
The percentage of positive coronavirus tests has also been rising.
In the seven-day span ending Thursday, an average of 11.2% of polymerase chain reaction, or PCR, tests performed each were positive, up from 9.3% the previous week.
Over the same period, the percentage of positive antigen tests rose from 18% to 22.1%.
"That tells us that there are a lot of cases, and in order to find all the cases, we need to do more testing," Dillaha said.
Hutchinson has said he wants to keep the percentage of PCR tests that are positive below 10%.
"I think that the Thanksgiving holiday is beginning to show the effects of the exposures that took place during that period of time," Dillaha said.
Dillaha said she was "a little heartened" by the drop in hospitalized patients, especially since she expects the spread of the virus to continue surging as people gather during the holidays.
"My concern is that people will not be conservative, that they'll want to continue their holiday activities, gatherings and events related to the holidays, and that exposure risk will remain high because there's already so much covid-19 in the communities," Dillaha said.
PRISON OUTBREAKS
The cases that were added to the state tallies included 2,188 confirmed through PCR tests.
The other 639 were "probable" cases, which include those identified through less-sensitive antigen tests.
The state's cumulative count of cases rose to 167,137.
Washington County had the most new cases, 260, followed by Benton County with 228, Pulaski County with 210, Craighead County with 146 and Saline County with 117.
Among prison and jail inmates, the Health Department's count of cases rose by 38.
State Department of Corrections spokeswoman Cindy Murphy said cases among inmates rose by 11, to 863, at the East Arkansas Regional Unit near Brickeys and by three, to 218, at the Tucker Unit in Jefferson County.
Of those cases, 45 at the Tucker Unit and 20 at the East Arkansas Unit were active as of Friday.
The state death toll rose by 27, to 2,370 among confirmed cases and by four, to 216, among probable cases.
Among nursing-home and assisted-living facility residents, the count of virus deaths rose by 20, to 1,098.
The number of people who had ever been hospitalized in the state with covid-19 rose by 123, to 9,329.
The number of virus patients who had ever been on a ventilator rose by nine, to 1,034.
PARKS ADJUST
In response to the rise in cases, the state Department of Parks, Heritage, and Tourism's Arkansas Parks division announced that it will limit hours at visitor information centers and museums, reduce seating capacity at restaurants in parks and restrict service at the marinas at DeGray Lake Resort State Park and Lake Ouachita State Park.
The information centers and museums will be open five days a week, "focusing on staying open during busiest days," the division said in a news release.
Campgrounds, cabins and lodges will remain open.
"Flexibility is necessary during these unprecedented times," department Secretary Stacy Hurst said in the release.
"Due to the impact of COVID-19 on our parks system, we must make adjustments in order to ensure that our most-used amenities and facilities continue to be available to the public during the days and hours they use them the most."
Meanwhile, a Pulaski County Quorum Court staff member's positive test for the virus last weekend, along with the rise in cases in the county, prompted the court to go to virtual meetings for the rest of the year.
Justin Blagg, director of the Quorum Court services, said the staff member was not feeling well just before Thanksgiving and tested positive the weekend after.
He said the court's office closed this week and will reopen Monday.
FEWER BEDS AVAILABLE
On Friday, 2,268 hospital beds -- 30 fewer from the previous day -- were available out of 8,963, meaning 75% of the beds are full, according to Health Department data. (Total beds include a few hundred in psychiatric or rehabilitation facilities that are not used for covid-19 care.)
Out of the state's 1,166 intensive-care beds, only 76 -- or 6.5% -- remain available. ICUs had 360 covid-19 patients as of 2 p.m. Friday, down from 375 on Thursday.
The state's total bed capacity -- hospital beds that can be staffed whether or not they are occupied -- dropped to 8,791 Friday, a drop of 10 from Thursday.
Total bed capacity has dropped by 2.5% since the end of November, going from 9,017 down to 8,791. Likewise, maximum flex bed capacity dropped by nearly 1.3% during the same time frame -- going from 11,351 to 11,204.
Out of the state's 1,053 ventilators in inventory, 663 -- or 63% -- remain available. There were 177 patients on ventilators as of Friday.
Chris Durney, a spokesman for the Central Arkansas Veterans Healthcare System, said John L. McClellan Memorial Veterans Hospital in Little Rock has 33 ICU beds and 11 covid-19 patients.
The number of ICU beds constantly changes in hospitals, he said.
There were four covid-19 patients at the hospital in regular beds as of Friday, Durney said. The number of those beds as well change frequently.
"Any room that covid patient has been moved to has been retrofitted to handle the covid patients," he said. "It's got negative air pressure and it goes through all the normal protocols. It is staffed, stocked with PPE and all of that."
STAFFING STRAIN
Shortages of health care workers have always been a struggle for hospitals, but the pandemic -- and all the extra duties it brought with it -- make the challenge even more pronounced, say hospital administrators across the state.
"It is very common for health care systems to have a staffing shortage and one that we deal with on a daily basis," said Cathy Dickinson, chief human-resources officer for Baptist Health. "What is different now is that most hospitals are trying to also expand hospital beds, specifically intensive care beds, to accommodate more patients. All of this is at a time when we already have a shortage in caregivers."
Trenda Ray, chief nursing officer and associate vice chancellor for patient care services at UAMS Health, said recruiting staff in the time of covid-19 is definitely more difficult.
"Nurses are making decisions not only professionally about where they want to work but also navigating the issues around virtual school and other family challenges everyone is facing during the pandemic," Ray said. "Applicants have withdrawn their applications when they learn they might care for covid patients."
Qualenta Forrest, vice president of human resources at CHI St. Vincent, said that while staffing has always been a struggle, the primary challenge now is the lack of ability to predict the impact of covid-19 on staffing levels.
"If an employee has to self-quarantine due to a possible community exposure, then identifying someone with the same skill set and experience to temporarily fill that role is a challenge," Forrest said.
Mitchell Nail, spokesman for St. Bernards in Jonesboro, said the pandemic and high community spread in the northeast region of the state has led to a number of team members isolated or quarantined.
"Many patient care staffers have worked additional hours and days to compensate, but we realize they cannot continue doing it long term," Nail said. "Knowing these challenges could likely present, St. Bernards has prioritized since the beginning of this pandemic that team members protect themselves both at work and within the community."
Charlotte Rankin, chief nursing officer at Mercy Hospital Northwest Arkansas in Rogers, said the pandemic has also impacted the method of recruiting, making it more difficult. In the past, hospital recruiters would visit schools and hold recruitment fairs.
"We are recruiting more virtually than in person," Rankin said. "We only had one recruitment fair since March to recruit nurses."
Dr. Steve Goss, president of Mercy Clinic in Rogers, said things are "about the same" from a recruitment standpoint, "no harder, no easier."
"We are more careful with in-person interviews when and if held, obviously," Goss said. "It is always a nationally competitive market."
Nail said the sense of urgency to fill open spots is much higher now.
"Covid-19 has forced us to approach nearly every aspect of health care differently, including hiring additional help," Nail said. "For example, we have accelerated our hiring process, decreasing the amount of time from application to start date."
Added to the staffing challenges is ensuring the health and well-being of staff members, Forrest said.
"Now more than ever, our health care support teams, including human resources, are focused on ensuring that our staff are being provided care as well," Forrest said. "That includes identifying talent to fill temporary and permanent open roles, develop and provide resources that address wellness, stress and other related material, in addition to the normal day-to-day partnership that we provide to help support and retain our staff. Our key focus is caring for our people."
PASTOR'S WIFE DIES
Maggie Chandler -- a pastor's wife, mother, author and former assistant to former Gov. Mike Huckabee -- passed away Tuesday after battling covid-19, according to Ben South, associate pastor of Central Baptist Church in Conway.
Chandler, 71, was the wife of the church's pastor, Don Chandler. They had been married 53 years.
"Maggie was a person who loved genuinely. It was from her faith in Jesus Christ that this love came," South said. "She was a faithful, consistent pastor's wife who treasured Scripture deeply."
About 25 church members tested positive for the virus over the past few weeks, South said. The Chandlers' daughter is in ICU with covid-19.
The congregation recently switched to virtual services only.
Huckabee said he and his wife, Janet, are "heartbroken" over Maggie Chandler's death.
Maggie was one of the original members of his team at the governor's office, Huckabee said by text message, but he had known her since the early 1970s.
"She was such a gifted writer, but beyond her many talents was her Godly spirit and her genuine compassion for everyone she encountered," Huckabee said. "She was beloved by all and disliked by none. She was humble and thoughtful, and had a true instinct to sense the pain of others and offer support and counsel."
According to her obituary, Maggie Chandler also took part in television shows for LifeWord Broadcast Ministries. She wrote a weekly column for the Baptist Trumpet newspaper and wrote several books.
The news of her death has been "stunning and a harsh reminder of the seriousness of Covid and that we are all susceptible to its scourge," Huckabee added.
Information for this article was contributed by William Sanders of the Arkansas Democrat-Gazette.