In December 2008, the Jonesboro trees were bowed and cracking with ice; a winter storm had swept through the city and left roads slick, but Tina Light decided to drive to her friend's house anyway.
The street proved too slippery.
Light's car hit another vehicle head-on, and Light landed in the hospital. She didn't go back to work for about two weeks. Her memories of that time are fuzzy -- she knows it was almost Christmas, that her family was out of town and that Engine 5 responded.
Light, then 38, doesn't know how long she stayed in the hospital nor have details of what she was doing. Her emotions and many thoughts for the next two years are lost because she doesn't remember. After the accident, she said, she started exhibiting signs of mental illness.
"When you have your whole life flash before you, it changes you," said Light, now 47.
After two years of dealing with mental illness without any treatment, she finally went to a mental health specialist. She came out of the meeting with a diagnosis of schizophrenia, a mental illness characterized by delusions, hallucinations and scattered thought patterns.
"Initially, it was scary," Light said. "To me, honestly, it was like having a death sentence, because I thought I'd lost the life that I had, that I'd lost a life that I could ever have moving forward."
But her community and family were supportive, and that support has helped carry her through, Light said.
After her diagnosis, she had to wait 4½ weeks to see a therapist.
Light's situation isn't unusual. Patients throughout Arkansas are often on hold for weeks between an initial diagnosis and the start of therapy or any medication adjustments, say advocates and former patients.
Psychiatrists, who are licensed to prescribe medication, have too many patients and too little time. There are slightly fewer than three psychiatrists per 10,000 residents in the state, according to the Bureau of Labor Statistics.
The National Alliance on Mental Health estimates that 20 percent of adults in the United States suffer from mental illness.
Most individuals under psychiatric care are on weekly, biweekly or monthly schedules. Those who are "stable" may see psychiatrists only every three months, mental health experts report.
Mental health practitioners in the state are trying new methods, such as telemedicine, to bridge the gap between the number of people needing care and the limited number of psychiatrists.
PRIMARY CARE
Some patients with mental illnesses turn to primary-care physicians for medication management as a way to forgo any delay in treatment.
While such physicians are licensed to prescribe medication and are often the first line of defense for someone going into crisis, they are not specialists, said Diane Skaggs, executive director of the Mental Health Council of Arkansas.
"If you've got somebody that's got a chronically mentally ill diagnosis, medically fragile, or the regular medications don't work, or if it's a child that needs ADHD medicine, you want to go to a specialist," she said. "And that's how we see psychiatrists. They're our specialists in brain work."
Thomas King of Fayetteville said his primary care physician was the first doctor to notice his depression last year.
King moved to California when he finished high school in 2004 to work on oil rigs and felt isolated from the rest of his crew. That's when suicidal thoughts started, he said.
He would imagine what it might feel like to drive off the road, picture his truck rolling cab-over-tire into a field.
When he was 20, after some tumultuous family experiences, he got the words "Hate Me" tattooed on his arm in dark block lettering.
"I felt like life would be easier if people didn't love me," he said. "I wouldn't disappoint them or anything like that."
When he moved back to Fayetteville and started dating his current girlfriend, she persuaded him to get help after his near-suicide attempt in 2016.
"I wouldn't say I attempted suicide, but I wouldn't say I didn't attempt suicide," King said.
The next time he saw his primary care physician, near the end of their meeting, he told her that something wasn't right. His depression was quickly becoming debilitating.
His doctor connected him with his "head shrinker," a psychiatrist at a community mental health center in Fayetteville, and things started to look up.
COMMUNITY CARE
Community mental health centers -- which serve specific regions of the state and provide services based on income levels -- are understaffed.
Arkansas began relying primarily on community-based mental health after state-run mental hospitals fell out of federal favor in the 1960s. Such hospitals across the state closed. There is only one left in Little Rock, which houses a couple of hundred people, a far cry from the nearly 3,500 it once served, Skaggs said.
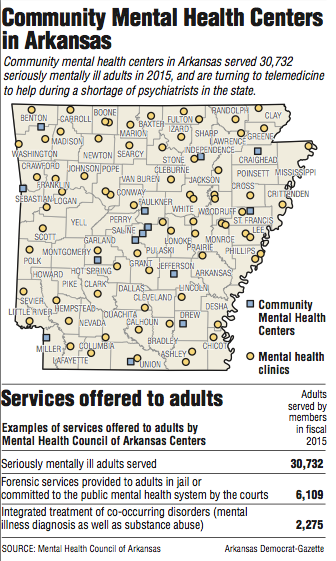
Arkansas' 15 community mental health centers served 30,732 "seriously mentally ill adults" in 2015. They also provide services to children and people who are incarcerated.
Each center has at least one main clinic. Some have smaller clinics, as well, but these are sometimes not staffed by anyone licensed to prescribe medication.
This is particularly prevalent in rural areas, where psychiatrists drive from larger cities to small clinics to see patients.
Dr. Benjamin Nimmo, a psychiatrist who works at Pinnacle Pointe Behavioral Health in Little Rock, said he works in Conway, Fordyce and Pine Bluff.
He used to work at a clinic in Magnolia. On those days, he spent more time in his car than he did seeing patients.
The system seemed unsustainable.
In 2010, the University of Arkansas for Medical Sciences received a grant from the federal government's Broadband Opportunities Program to start telemedicine programs.
UAMS started with 456 participating sites for telemedicine, and several community health centers also jumped on board, said Alan Faulkner, the director for the university's broadband program.
TELEMEDICINE
A telemedicine meeting with a psychiatrist works much the same as an in-person visit. A nurse starts the session and steps out of the room. The client is then left to chat via web camera with the provider.
The computer screen must be at least 20 inches diagonally, and insurance companies have minimum requirements for Internet connectivity, which Faulkner helps sites set up.
Cameras have the capability to zoom in on clients to read facial expressions or see if the client is exhibiting any abnormal behavior.
Mid-South Health Systems in Jonesboro was one of the first clinics in the state to start using telemedicine for behavioral health. Clinicians do not use telemedicine for talk therapy, only for medication management, said Roland Irvin, the system's chief operating officer.
The Jonesboro-based system serves 13 counties and has telemedicine services in Marianna, Brinkley, Forrest City, Wynne, West Memphis, Blytheville, Paragould, Pocahontas and Corning, Irvin said.
Mid-South began telemedicine services 11 years ago when Medicaid began allowing billing for the service. More than half of community health providers' clients use Medicaid.
In Northwest Arkansas, the Ozark Guidance Center started using telemedicine about five years ago, Executive Director Rusti Holwick said.
Like the Jonesboro clinic, Ozark Guidance uses it mostly for primary assessments and medication management, Holwick said.
Both sites also can assess via webcam people who enter the emergency room and are in mental health crises. Whereas previously doctors on call may have had to drive to two or three emergency rooms in a night, they can now potentially see all the clients from their home offices.
This may not work for all patients, something Irvin said his office is working to rectify.
Patients "might have some ideas about what's going on with that television that are not rational," he said. "But most people in a mental health crisis are glad to get to talk to somebody as quickly as possible, even if it means that they're speaking to them over the television."
Kathy Harris, the president of the Southeast Arkansas Behavioral Health Center in Pine Bluff, said her center now uses webcams for doctors to see prisoners, particularly those in the nearby juvenile jail.
This frees officers from having to transport inmates to the center for therapy and shortens the wait for treatment, Harris said.
"Just because they step into a detention facility, they should not lose the access to the care that they needed," she said of prisoners.
Treating mental health issues remotely is growing rapidly.
Holwick said her office is exploring the idea of having a telecourt system in which a judge could speak with an inmate and a psychiatrist to make decisions about cases.
In Pine Bluff, the center started virtually treating several patients in Sheridan just a couple of months ago, Harris said.
UAMS' telemedicine services are expanding beyond the field of behavioral health to encompass dermatology, obstetrics and even treating hand injuries, Faulkner said.
While all of the centers have experienced some resistance from patients, doctors or other partners in implementing telemedicine services, proponents say it is the best solution to the shortage of psychiatrists.
"I think the thing to understand is ... the option is between telemedicine service and receiving no service," Nimmo said.
SundayMonday on 11/26/2017