The state's largest public employer is cutting 600 positions, nearly half of which were filled, in an effort announced Monday to curb a deficit almost double the amount it initially budgeted.
The layoffs make up about 2 percent of UAMS' total 10,900 employees across the state, while the overall cuts -- including vacancies -- make up 5.5 percent of the academic medical center's workforce. The positions are across all areas and will take effect in either 30 or 60 days, depending on the employee's contract, said Leslie Taylor, UAMS' vice chancellor in the Office of Communications and Marketing, who called the move "a very difficult decision."
"UAMS is all over the state, and we work and manage programs that people aren't even aware of," she said. "We have a $3 billion economic impact and are the largest public employer in the state. We're just trying to find the right balance with our size and with our programs, so that we're making sure that we deliver the best value for people in the state of Arkansas."
UAMS administrators said they tried to minimize any effects to its three-pronged mission -- educating health care professionals, providing patient-centered health care and advancing research -- but Taylor did not know Monday whether the cuts would trickle down to affect services. She added that patients should not feel any of the repercussions due to the layoffs and vacancies.
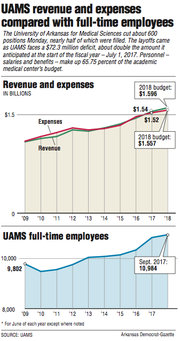
The cuts come as UAMS faced in the first quarter of this fiscal year -- which started July 1, 2017 -- a deficit of $72.3 million, nearly twice as much as the $39.8 million deficit the University of Arkansas trustees authorized the institution to carry back in May. The deficit doesn't concern how much cash it has on hand but represents a decline in net assets, which comprise revenue, expenses, depreciation, investment income and other funds.
Personnel -- including salaries and benefits -- makes up 65.75 percent of UAMS' $1.5 billion budget, according to UAMS. The academic medical center said it expects the cuts in positions to save between $26 million and $30 million in the fiscal year that ends June 30.
"Our productivity, we don't believe, is our primary issue," said Stephanie Gardner, UAMS' interim chancellor. "Our hospital is full. But we need to change the expense curve, and, to some extent, we're going to have a lot more pressure on the other parts of our mission."
The number of full-time employees has increased by 9.1 percent since June 2013, she said, but it has done so at a time when UAMS has added academic programs, grown in its research enterprise and opened new clinics to better serve the state, Gardner said.
"So this number looks like a big increase," she said. "It has impacted our expenses, but, at the same time, it's a reflection of a lot of our growth."
Many academic medical centers nationwide are facing similar financial conditions, experts say.
"Across the country right now, there has been certainly two major organizations or major fields that are under intense scrutiny and financial pressure: health care and education," said Dr. John Prescott, the chief academic officer at the Association of American Medical Colleges in Washington D.C. "So, the combination is especially difficult for those who are in academic medicine."
All health care providers are facing challenges, in part because they are providing very expensive tertiary care -- very sophisticated care, such as transplants or heart surgeries -- and getting "less generous rates" from payers, said Michael Chernew, the Leonard D. Schaeffer Professor of Health Care Policy and director of the Healthcare Markets and Regulation Lab in the department of health care policy at Harvard Medical School. Academic medical centers have an extra arm of teaching, he said.
Many health care providers, including academic medical centers, have not historically focused on efficiency of health care delivery, Chernew said, adding that, in the past, academic medicine has homed in on their missions.
"They got used to high prices," he said. "They built a lot of stuff."
Now, though, there's a broad societal debate about who is willing to pay how much for high-quality physicians, Chernew said. People are not used to talking about health care as a business, but it's starting to look more like a business, he said.
Other changes at the federal level make the future of health care even more uncertain.
In Arkansas, UAMS has increased revenue, in part because of a reduction in uncompensated care, a result of Arkansas Works, the state's expanded Medicaid program. But the state has requested federal approval to move about 60,000 people off the program by limiting eligibility to people with incomes up to the poverty level, instead of 138 percent of poverty level, and to impose a work requirement on many of those remaining. As of Monday, the state had not received word on approval of the waivers.
One of the biggest challenges that academic medicine is facing is continued funding for the future, Prescott said.
But that doesn't spell out their ending, Chernew said.
"I do not think that there's someone coming over the hill to send more money," Chernew said. "They've got to adapt to new realities to survive. They're going to make sacrifices in mission, manage their costs aggressively and raise tuition. One way or another, they're going to have to make their business model work."
Nearly three-quarters of UAMS' budget comes from the clinical enterprise, while only 6 percent comes from the state and about 3 percent comes from tuition, said Bill Bowes, the academic medical center's senior vice chancellor for finance and administration and chief financial officer. The remainder is made up of capital gifts, federal grants and contracts, among other things.
Its state appropriations peaked in fiscal 2014 at about $120 million, but that amount has dropped to about $107 million-$108 million annually over the last few years, Bowes said. About $21.5 million of state appropriations are "pass-through or designated funds," leaving UAMS with $86 million.
On top of that, UAMS shells out a varying amount annually for a Medicaid match, Taylor said. In fiscal 2016, after the match, UAMS had a net state appropriation of about $8 million to operate its hospital, academic and research arms. The next fiscal year, UAMS' net state appropriation was $31 million, she said.
The state, unlike some of its peers, otherwise does not fund UAMS for teaching future medical professionals. As an example, South Carolina funds both the Medical University of South Carolina along with its hospital, a separate entity.
State Sen. Larry Teague, D-Nashville, said Monday that he had not been briefed on the academic medical center's budget yet, but he said that UAMS has asked "consistently" over the last four or five years for more money.
"We have strung them out," said Teague, co-chairman of the legislative Joint Budget Committee. "We've not really given them a lot of help, so we're probably reaping somewhat what we sowed."
Gov. Asa Hutchinson acknowledged that state funding for UAMS has been steady since he took office and he has previously supported UAMS with additional resources. But he said Monday that, at this point, "there are no current plans for additional general-revenue assistance from the state."
The governor plans to present his general revenue budget to the Joint Budget Committee today.
At the end of the first quarter of this fiscal year, UAMS was $72.3 million in the hole, in part because of $17.5 million in unfunded budget initiatives, said Gardner, the interim chancellor. The clinical enterprise -- which subsidizes other parts of the academic medical center -- was also running about $15 million short of what was originally budgeted.
"We didn't get here over the last three months," she said. "This has actually been a trend over the last several years .... So, our revenue has steadily increased over the last almost 10 years, but our expenses have also continued to increase."
Revenue actually increased from last year, but it hasn't done so at the anticipated rate of 6 percent, she said. So far, it's grown by a meager 2 percent to 3 percent.
The academic medical center begins a new alliance with Baptist Health, starting this year. The alliance will help the two coordinate care for some 50,000 Arkansans on Medicare: the health care providers will have a "more complete picture" of patients' health and deliver the right care to them at the right time, according to UAMS and Baptist Health.
If the two institutions are able to save money through a reduction in service use, the pair will be able to share in those savings.
The two -- along with Arkansas Children's Hospital, Arkansas Blue Cross and Blue Shield and Fort Smith-based Bost Inc. -- have also formed the Provider-owned Arkansas Shared Savings Entity, a way to manage Medicaid costs for eligible patients with behavioral health disorders and development disabilities.
Both of those required each entity -- including UAMS -- to put up initial funds "as a reserve against loss," Bowes said, adding that the two totaled about $3.5 million for the academic medical center.
UAMS wanted to take part in both to move in the direction that health care is going: population health management strategy, Gardner said.
"These are early opportunities for us to gain experience with these strategies that are relatively low risk, she said. "And, I think, if you look at down the road, what we're hoping -- like two or three years out -- is that we're going to accomplish shared savings. So these are focused on what should be a positive for our bottom line in the future and also help us gain experience to be able to expand to do this with other populations."
UAMS also had a $5 million difference between where administrators thought Medicaid supplemental payments would be and where they actually were, and it is not expecting that to occur again, she said.
Because of the deficit, UAMS instituted a review by senior leadership of all vacant positions before departments could hire and put an end to position reclassifications and out-of-cycle salary increases. Those -- which started about mid-November -- will continue after the 600-position cut, Taylor said.
UAMS brass would dole out those salary increases, at times, to make market adjustments in specific fields but, more commonly, when another institution courted an employee, Gardner said. The academic medical center has spent about $8 million annually in re-classifications and out-of-cycle adjustments, she said.
UAMS has not had layoffs before, though, in 2009, when former Chancellor Dr. Dan Rahn started and brought in consultants to help create efficient practices, it trimmed "a couple hundred" positions -- mostly in the hospital area -- over time through attrition, including retirements and people leaving for other jobs, Taylor said.
Rahn, who retired in July after nearly eight years as chancellor, managed to cut UAMS' budget by $120 million over his tenure and increased operating revenue by more than 40 percent.
This go round, 258 people lost their jobs, while the remainder were vacant positions. Taylor did not know the complete picture Monday of which layoffs or vacancies came from which region of the state, nor did she have a full breakdown of the types of jobs in the mix.
In Northwest Arkansas, though, UAMS cut 6.5 positions. Two of the positions were already vacant. Another two were part of an exercise to create efficiencies in its electronic health record and were notified in August that their positions would end in April. Yet another two were notified Monday, and one person was moved to a part-time basis.
She added that about 40 positions -- it was unclear how many were already vacant -- came from Children's Hospital, which is based in Little Rock. UAMS pediatricians and physicians provide care at Children's Hospital.
In a previous interview, when asked about potential cuts to academics and unfunded research, Gardner said repeatedly that "everything is on the table." Senior leadership also suspended budget conferences typically held in February and March, she said, instead focusing on short- and long-term strategies.
UAMS has created an email address for employees to suggest other ways to save money, and senior leadership is reviewing those recommendations. It has already held a town hall-style meeting to discuss its fiscal situation with employees.
"Where this leaves us now is we need to recognize the fact that academic health centers across the country are having many of the same challenges, but we can't sacrifice our mission of providing health care in the process," she said. "We have to recognize that we have an operational model that's not sustainable, that everything's on the table, that we have to look at every aspect of the services and programs that we're offering and determine what's critical and what's sustainable."
A Section on 01/09/2018